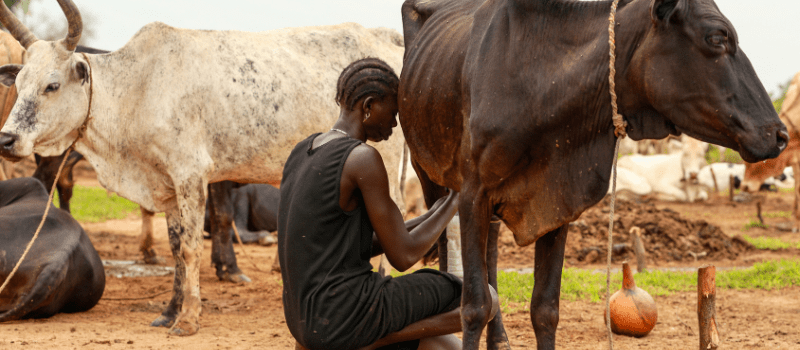As VWB joins the global call of the International Year of Rangelands and Pastoralists (IYRP 2026) and the Healthy Rangelands Manifesto, Janine Mitchell, Executive Director of Veterinarians Without Borders North America (VWB), reflects on what mobility-first animal health means in practice.
Mobility is often misunderstood.
In rangelands and remote landscapes, movement is not a sign of instability or underdevelopment. It is a sophisticated strategy for living with variability — following pasture and water, reducing grazing pressure, managing seasonal risk, and sustaining livelihoods where change is constant.
This year is the International Year of Rangelands and Pastoralists (IYRP 2026). We invite the world to take rangelands seriously, and to recognize pastoralists as essential stewards of landscapes that matter for food systems, biodiversity, and climate resilience. For those of us in animal health, IYRP 2026 surfaces a design challenge we can’t ignore. If people and herds move, services must move too.
The real barrier isn’t mobility. It is access.
In many countries, veterinary systems still assume a fixed world. These fixed clinics, fixed catchment areas, fixed schedules, and fixed supply chains can work well for settled communities. In rangeland and remote contexts, they too often fail by design. When care stays put and communities move, the result is predictable. Preventable disease will persist, outbreaks are detected too late, herd productivity declines, and the communities most reliant on livestock are least able to access reliable services.
 PHOTO: Cattle herders guide their herd across grazing land in Aweil East, Northern Bahr el Ghazal State, South Sudan.
PHOTO: Cattle herders guide their herd across grazing land in Aweil East, Northern Bahr el Ghazal State, South Sudan.
This is frequently described as a “hard to reach” problem. But that framing blames geography and lifestyle rather than systems design. Pastoralists and remote communities are not inherently hard to reach. Our models are just often hard to move.
At VWB, we think the shift required is straightforward, but by no means simple. We aim to build mobility-aware animal health systems that match the realities of distance, seasonality, and movement.
What does “veterinary care that moves” actually mean?
It is common to equate mobile veterinary care with a vehicle, a temporary clinic, or a one-off outreach trip. Mobility-aware care is more than a visit or a clinic day. It is a connected system designed to make access reliable, safe, and sustainable.
In practice, veterinary care that moves is designed for both pastoralist and remote communities where distance, seasonality, or limited infrastructure make routine access to care unreliable. It starts with outreach services planned around where people and animals actually are, whether that means seasonal movement routes or communities that may go months or years without a visit. It pairs those visits with community-based animal health capacity so support continues between trips, backed by supply chains and quality assurance systems that work in low-resource settings.
It also depends on communication and surveillance tools that function off-grid and connect frontline information to timely response, all supported by partnerships and governance that align across communities, routes, and institutions.
Mobile care in places where the clinic doesn’t exist
In northern Canada, many remote communities do not have permanent veterinary clinics. Some may wait months, or even years, between visits. This gap creates real risk, including in places where rabies is present and unvaccinated animals can carry serious consequences for both animals and people.
VWB’s Northern Animal Health Initiative (NAHI) was created in response to community invitations and built around a One Health approach: meet communities where they are, strengthen local capacity, and deliver services in ways that work in the North.
 PHOTO: VWB’s Northern Animal Health Initiative (NAHI) team provides vaccinations and wellness care during a community clinic in Fort Liard, Northwest Territories.
PHOTO: VWB’s Northern Animal Health Initiative (NAHI) team provides vaccinations and wellness care during a community clinic in Fort Liard, Northwest Territories.
NAHI is built around the reality of northern access. Reaching communities may require travel by ice road, bush plane, or boat. When you treat that as the baseline rather than the exception, you can plan services, staffing, and logistics accordingly. NAHI also treats mobility as an opportunity to build continuity, not a reason for episodic engagement. Telehealth support and community training help extend the impact of short visits. It’s not “a clinic and goodbye.” It’s a relationship, and a system.
Our model is rooted in trust and co-design. In Indigenous northern communities, trust comes first. It shapes whether services are welcomed and used early enough to prevent problems from escalating. NAHI shows that geography does not have to be the limiting factor when services are built for proactive outreach and consistent follow up.
When access is scarce, local providers become the system
Mobility and access constraints do not always come from geography alone. In some settings, the limiting factor is capacity, where demand far exceeds the available professional veterinary workforce.
Ghana’s Upper East Region is home to 1.3 million people and over 3 million livestock, where there are only six licensed veterinarians. Each veterinarian covers enormous distances, supported by a limited number of animal health officers. In that context, expecting clinic-based systems to reach every community is unrealistic.
So, communities do what they’ve always done. They adapt. The question is whether systems support that adaptation with quality training, and strong links to formal veterinary oversight. VWB’s partner, the Ghana Poultry Network (GAPNET), has trained more than 90 Community Animal Health Workers (CAHWs), 70% of them being women, to extend care to remote farms. This model closes access gaps by shifting care to the community level and enabling faster response. CAHW’s can deliver routine prevention and basic treatment such as vaccinations, deworming, and minor wound care, which reduces avoidable losses and helps identify problems earlier.
 PHOTO: GAPNET-trained Community Animal Health Workers (CAHWs) use a mobile reporting tool to document a young goat’s illness for a local farmer in Ghana’s Upper East Region.
PHOTO: GAPNET-trained Community Animal Health Workers (CAHWs) use a mobile reporting tool to document a young goat’s illness for a local farmer in Ghana’s Upper East Region.
It also allows professional veterinary support to be used where it is most needed, with veterinarians focusing on complex cases and higher risk situations instead of being stretched thin across routine needs. Because CAHWs are known in their communities, trust also strengthens, and that trust improves uptake, especially for prevention.
What makes this mobility-aware rather than simply decentralized is that care follows where people and animals actually are. CAHW’s are moving from compound to compound, meeting farmers in their daily reality, and operating in settings where a fixed service point may be a full day’s travel away.
Importantly, this model can also strengthen surveillance. In the Ghana work, CAHWs use FAO’s Event Mobile Application (EMA-i) to record and report illness and potential disease events. This links frontline observation to national animal health systems. This is a powerful example of modern One Health infrastructure operating from a village path.
Mobility-first animal health is resilience infrastructure
A common concern is cost. Mobile clinics, outreach, training, supervision, and the supply chains that keep services reliable can look more expensive than a single fixed facility line item. That comparison is misleading. The real question is not whether mobile services cost more than a building, but what systems cost when prevention is inconsistent, when detection comes too late, and when households face avoidable losses that compound with every shock.
Mobility-first animal health systems shift the balance toward reliable prevention instead of recurring and preventable loss, and toward early detection and response instead of late crisis management. They support household resilience by reducing the cycle of shock and recovery, and they advance equity by reaching communities that are otherwise structurally excluded from routine care.
 PHOTO: A livestock keeper stands with her cattle during a VWB-supported vaccination campaign in Northern Bahr el Ghazal State, South Sudan.
PHOTO: A livestock keeper stands with her cattle during a VWB-supported vaccination campaign in Northern Bahr el Ghazal State, South Sudan.
The value of mobility-aware systems is often easiest to see when it is missing, because it shows up in what does not happen. Fewer animals die from preventable causes. Productivity improves as animals stay healthier for longer. Outbreak impacts are reduced because warning signs are noticed earlier and acted on faster. Food security strengthens when livestock assets are protected and households can rely on animal-source foods and income. Public health protection also improves in places where people and animals live closely together and risks at the animal–human interface are part of daily life.
Mobility-aware animal health functions as resilience infrastructure — as essential as roads, water systems, or communications. It protects the assets people rely on and stabilizes livelihoods under stress.
What IYRP 2026 should push us to do differently
IYRP 2026 is a spotlight, and the real question is what we do with it. From VWB’s perspective, this year should help shift how animal health systems are designed and funded so they reflect the realities of rangelands and remote settings rather than an idealized, settled world. Mobility is normal. Seasonality is normal. Distance is normal. Systems work best when they are built for that baseline, not for the easiest month of the year when roads are passable, animals are nearby, and travel is simple.
It should also push us to invest in the behind-the-scenes foundations that make access reliable. Training matters, but it is not enough on its own. CAHW’s and mobile service delivery only work when they are supported by consistent supervision, clear referral pathways, dependable supplies, quality assurance, and information systems that lead to timely response. These elements are not always the most visible part of a program, but they turn short-term outreach into a durable system that communities can rely on year after year.
Above all, IYRP 2026 should reinforce that communities are not just recipients of services. They are co-designers of what works. Mobility-first systems succeed when they are built with local leadership, local knowledge, and local accountability, and when trust and legitimacy are treated as essential rather than optional. That is what determines whether prevention practices take hold and whether early warning is shared and acted on in time.
 PHOTO: Three VWB-trained Community Animal Health Workers (CAHWs) travel to support a vaccination campaign in Aweil East, Northern Bahr el Ghazal State, South Sudan.
PHOTO: Three VWB-trained Community Animal Health Workers (CAHWs) travel to support a vaccination campaign in Aweil East, Northern Bahr el Ghazal State, South Sudan.
Movement is the blueprint
One final thought is worth holding onto. Movement is not the barrier. It is the blueprint. Pastoralists and remote communities have long developed strategies for uncertainty, and mobility is among the most effective — protecting land, herds, and livelihoods in environments that defy neat schedules.
If we design veterinary systems as if everyone is settled, we will keep arriving too late. If we design for movement — through mobile clinics, community-based providers, reliable supply chains, and connected surveillance — we can expand access in ways that are equitable, modern, and resilient.
That is what IYRP 2026 can mean for VWB. Veterinary care that moves can move health and livelihoods forward.

Movement is not the barrier. It’s the blueprint.
Join VWB and partners across the VSF International network in calling for stronger investment in community-led animal health systems that work for rangelands and pastoralist communities.